As Alzheimer’s disease continues to affect millions worldwide and effective treatments remain limited, scientists are exploring a bold new direction: repurposing cancer medications. Research is shedding light on the possibility that drugs originally developed to treat tumors might help slow, or even reverse, the cognitive decline associated with Alzheimer’s. This innovative strategy aims to accelerate treatment development and offer new hope for patients in need.
The concept behind this strategy is intriguing: numerous cancer treatments that have already been deemed safe for humans can swiftly proceed into Alzheimer’s clinical trials. These medications are being studied for their potential to affect biological processes involved in both cancer and Alzheimer’s—such as inflammation, protein misfolding, and altered metabolic pathways.
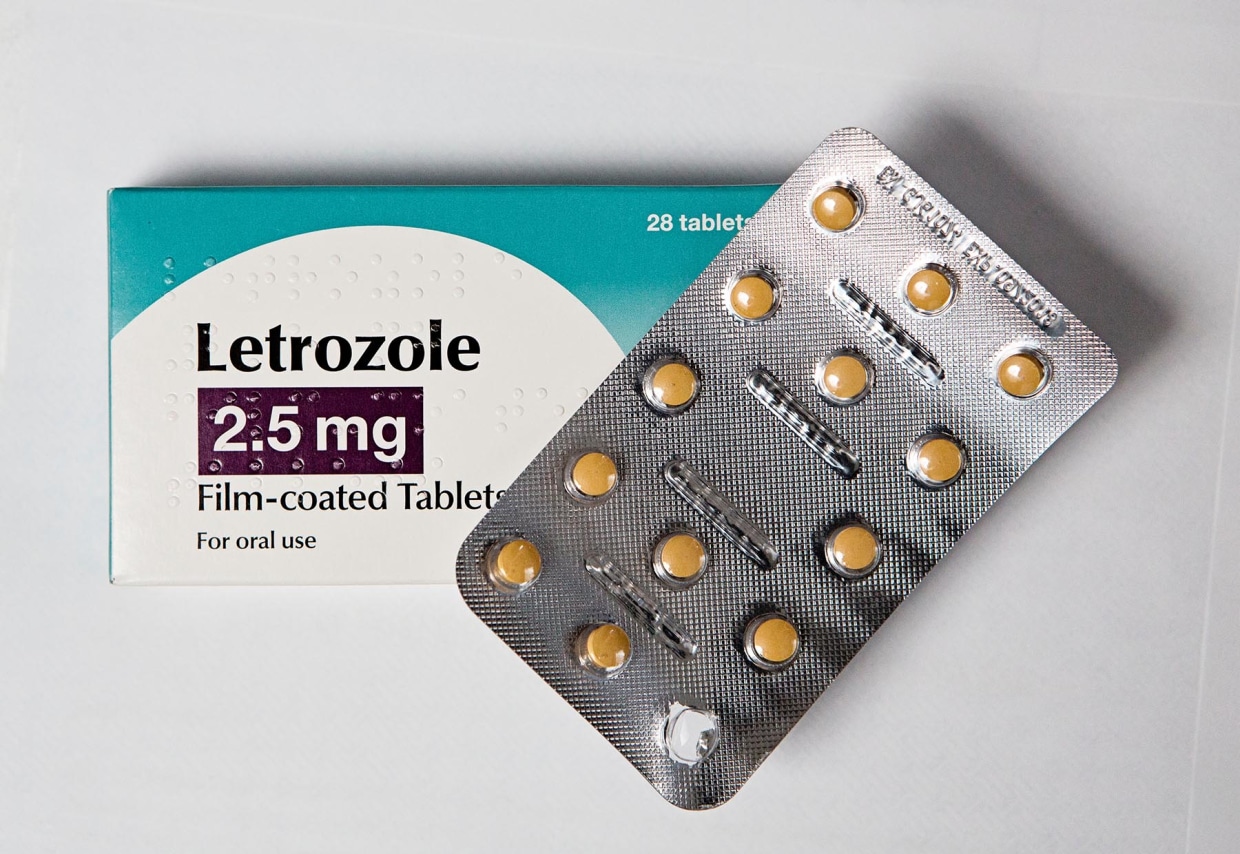
One notable instance includes medications such as letrozole and irinotecan, applied in the treatment of breast, colon, and lung cancers. In lab research, these drugs seemed to mitigate Alzheimer’s by altering detrimental gene expression patterns present in brain tissue. Studies on animals in preclinical stages indicated that a mixture of these pharmaceuticals decreased protein clumping, enhanced memory, and diminished neuron deterioration in Alzheimer’s models. Data from epidemiological observations also suggested a reduced risk of Alzheimer’s in older individuals who had been treated with these medicines, implying possible protective benefits in humans.
Research teams are still exploring tailored treatments like bexarotene and tamibarotene. These medications, originally intended for specific cancer forms, operate on receptors that control the clearance of proteins in the brain. Initial studies on mice have shown a decrease in amyloid plaques (a key feature of Alzheimer’s) and cognitive enhancements. Although the findings are encouraging, the long-term safety of these drugs in older individuals is still being carefully reviewed.
In an alternative approach, researchers examined saracatinib, a molecular inhibitor of kinase initially designed for cancer treatment. This compound exhibited potential in restoring memory and cognitive abilities in animal models of dementia. While it was not successful in cancer clinical trials, it displayed neuroprotective properties in Alzheimer’s studies and is currently under investigation in preliminary human trials to evaluate its tolerability and effectiveness.
Meanwhile, immunotherapy drugs known as IDO1 inhibitors—being evaluated for cancers like melanoma and leukemia—are emerging for their ability to correct disruptions in brain glucose metabolism in Alzheimer’s models. In mice, these drugs improved energy processing in crucial brain cell types and restored cognitive performance. This metabolism‑focused mechanism offers a fresh angle for treating neurodegeneration.
Experts suggest that Alzheimer’s and cancer share several underlying biological traits, including abnormal cell signaling, inflammation, vascular changes, and protein aggregation. By targeting pathways common to both diseases, cancer therapies may slow degeneration through mechanisms separate from traditional Alzheimer’s drugs, which largely focus on amyloid or tau proteins.
Several cancer drugs are already in clinical trials for Alzheimer’s treatment. These include kinase inhibitors such as dasatinib and bosutinib, immunomodulatory agents like lenalidomide, and histone deacetylase inhibitors. While some trials are still in early phases, others have completed testing in small groups, generating insights into safety and dosage.
Analysts warn that numerous cancer medications can lead to major side effects, which could be dangerous for elderly individuals or vulnerable patients. Issues related to the digestive tract, hormonal imbalances, and weakened immune systems are some of the concerns. As a result, scientists stress that repurposing these drugs should thoroughly consider advantages and drawbacks, beginning with closely observed trials and cautious dosage levels.
Still, the advantages of drug repurposing are hard to ignore: reduced development costs, established manufacturing processes, and tangible safety data can all help shave years off the pathway to patient access. Computational methods—combining gene expression profiling, big‑data mining, and patient health records—are accelerating the identification of promising candidates and optimizing trial design.
If even one of these cancer drugs proves effective and safe for Alzheimer’s, it would represent a substantial breakthrough. Unlike existing approved medications that only modestly slow cognitive decline, these therapies offer potential for actual repair of brain circuits and reversal of disease symptoms in early stages. For patients and families facing the emotional devastation of memory loss, that is profound hope.
Nevertheless, the journey from promising laboratory findings to proven human intervention is long. Alzheimer’s remains a complex disease involving multiple overlapping brain pathways. Researchers stress that a combination of drugs—and potentially pairing these with lifestyle or metabolic therapies—may be needed to attain meaningful outcomes. From diet interventions to immune modulation, future Alzheimer’s care could resemble a more holistic, personalized model.
In the broader landscape, the exploration of cancer medications may dovetail with other emerging strategies for Alzheimer’s: antibody treatments, novel small molecules targeting tau proteins, and even neuroprotective gene therapies. As researchers refine their understanding of disease mechanisms, combinations of approaches may offer the best chance for stopping or reversing cognitive decline.
The potential convergence of cancer and neurodegeneration research is reshaping how scientists think about Alzheimer’s treatment. What began as a desperate search for new drugs may lead to an entirely new way of tackling the disease—by looking to medications already on the market and redirecting them toward brain health. If this path leads to even modest reductions in Alzheimer’s progression or new treatment options, it could be one of the most transformative developments in decades.
Currently, clinical trials are either being conducted or are in the planning phase. The scientific community is maintaining a cautiously positive outlook. If present and upcoming research confirms tangible advantages for humans, it might signify a new chapter of repurposed therapies for Alzheimer’s—providing not only symptom control but a genuine improvement in cognitive resilience.
The question, “Could cancer drugs be the future of Alzheimer’s treatment?” is no longer speculative. It’s a line of inquiry generating tangible data and promising early results. With robust safety evaluation and rigorous trial design, this approach may help deliver novel therapies to millions of people living with Alzheimer’s—and those at risk of developing it.